Piedmont Hospital Gets Back to Business
After COVID-19 cases peak, surgeries resume at newly expanded Buckhead facility. But chief medical officer is prepared to reverse course if necessary.
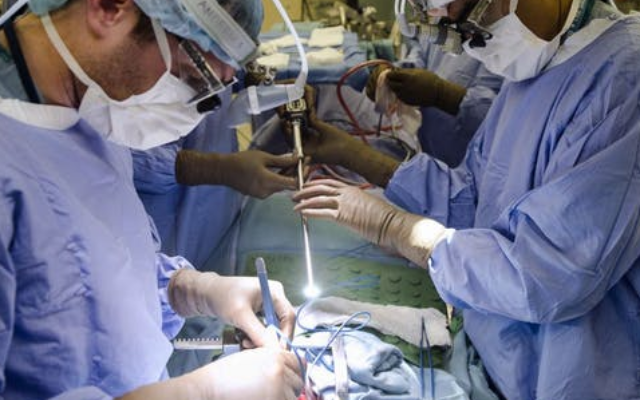
Initially struggling to cope with a rapid influx of coronavirus patients beginning in March, Piedmont Atlanta Hospital, like so many other health care facilities, is beginning to see patients in need of surgical procedures that can be scheduled in advance. Not only are the surgeries medically necessary, they’re an important part of the financial foundation of hospital care.
The American Hospital Association estimates that hospitals in America are losing more than $50 billion a month because of cutbacks in elective non-emergency procedures.
We spoke with Dr. Mark Cohen, chief medical officer at Piedmont, a 643-bed facility, including the recently expanded capacity of 100 new beds. He discussed challenges of balancing the need to do more elective surgery while remaining alert to the dangers of the pandemic.
AJT: Where are we now in terms of caring for those patients who need to be hospitalized for COVID-19 infections.
Cohen: So the peak here at Piedmont was in late April and the numbers have gone down. We’re down now maybe to 20 percent of where we were at the peak, which has enabled us to open up for our usual patient care. So we’re back to full operations, and doing all procedures and all admissions. But we’re monitoring the COVID census very carefully and prepared to start to cut back on the patient care we are doing now, again, if we need to.
One of the big questions is not knowing how far to go in doing elective and other surgeries. You don’t want to get yourself in a situation where you don’t have the capacity to deal with a sharp uptick in COVID cases and that sort of thing. Is that a difficult question for us? Yes, it’s a concern. But I think now, because of what we know about COVID, rather than unknowns as it was several moths ago, it’s a much less difficult question.
AJT: So if this crisis were to suddenly take off again, how would Piedmont react?
Cohen:When the epidemic first hit, all we knew was China, Italy and New York City. And those three were just totally overrun. Horrible scenes on television of New York City hospitals renting refrigerated trailers to put bodies in, staff with no personal protective equipment and no hope for getting it. So that was our model and we prepared for that.
What we’ve learned since is that if the volume of COVID cases increases, if opening in Georgia was too soon and social distancing fails, it’s not going to hit us as a crisis from one day to the next. It’ll be one week to the next. And that’s enough of a lead time for us to cut back on non-emergency surgeries and begin to create capacity again.

AJT: What do you think has been the impact of all of this on your staff and particularly your physicians and those on the frontlines of this?
Cohen: In the beginning we were scared. We were scared for ourselves and scared for our mission. We did not have enough protective gear to allow people to use N95 masks from the time they would come to work until the time they left. We had to restrict it just to exposure to high-risk situations. People felt the conflict of their usual mission, which is to take care of patients. But that sometimes conflicts with taking care of myself. So I’m going in to see a patient. Am I putting myself at risk and by extension, my family?
Those things were very much in conflict. So early on, people were scared. Some were angry. Some blamed us for no being better prepared than we were. And by now, three months out, people are pretty accepting. I think it’s almost at the point now where this is just part of our lives.
AJT: What has this crisis taught you about how you relate to your patients?
Cohen: Emotionally, for me personally, probably the hardest thing has been our no visitor policy. We’ve had to restrict a number of people in the building for safety and we have not allowed visitors. And I’m the one who grants the exceptions. And it got to the point for me, a couple of weeks ago, where I went to other members of my executive team and said, “I’ve had it, I need a break. I just can’t keep hearing the stories of the sadness of the patients and families that want to be been able to be together and having to tell them ‘no.’”
So we’re social organisms. We need to be together. I haven’t hugged anyone other than my wife in three months. I haven’t shaken hands with anybody. I mean, I never knew how important that was.
Note: Piedmont Hospital has updated its visitor policy. While COVID-19 patients are still not permitted visitors, most other patients are allowed one visitor during each 24-hour period, but only from 9 a.m. to 6 p.m. Full details are available at https://www.piedmont.org/locations/piedmont-atlanta/pah-visitors.




comments