Healthy Sleep Will Keep You Awake and Alive
Scott Greenhut's inspirational journey started when he was 32 and north of 300 pounds, and started with addressing his issues with sleep.
Nearly two years ago, just after the end of the high holidays, Scott Greenhut made a New Year’s resolution. He promised himself that he would do everything in his power to save his own life.
His father had died of kidney failure at the age of 62. His mother succumbed to cancer at 44. His sister was close to death in her mid-30s, and at 32 he felt like he was slowly dying. He had found it hard to stay away from the array of fried foods, sugary desserts and empty carbs at the buffet restaurant just behind his apartment off Pleasant Hill Road in Gwinnett County. All those meals of greasy calories and tempting sweets had pushed his weight past 270pounds.
He had no energy and he was always tired. He frequently felt like falling asleep in the middle of the day. Although he needed to lose the weight and eat better, his doctor advised him to start his road to sound health with a good night’s sleep.
According to Dr. Scott Leibowitz, past president of the Georgia Association of Sleep Professionals, sleeping well is seen as the foundation of a healthy lifestyle.

“In the last couple of decades, quite honestly, there’s been an explosion of interest in the field of sleep, in a large part because of our increasing knowledge of the impact of sleep. And health, in every sphere of essentially every human function, is impacted in some way by the way we sleep.”
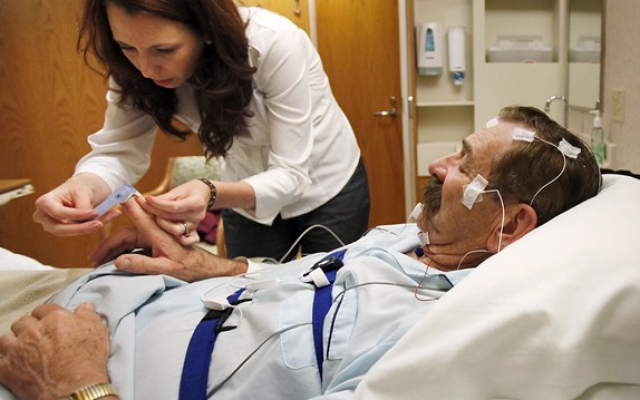
For Greenhut, the search for a sound night of sleep began with a fitful snooze in a sleep study lab. There, sensors attached to his body recorded his heartbeat and eye movements and the fact that his breathing stopped momentarily almost twice every minute he was asleep, 105 times an hour, a clear sign of a condition known as sleep apnea.
He was one of the estimated 22 million Americans with a condition that can cause a continuous but temporary obstruction in our breathing while we are asleep. The American Sleep Apnea Association reports that 80 percent of those with sleep apnea are unaware they have a moderate to severe case of the condition.
The simple solution for many of those like Greenhut, who are diagnosed with the problem, is a prescription for a Continuous Positive Airway Pressure machine, commonly called CPAP, a small air pump device attached to a face mask that fits over the nose and mouth. A constant flow of air, under moderate pressure, allows the breathing passages to remain open and keeps you sleeping soundly.
But for all those with serious untreated sleep conditions, including sleep apnea, the dangers are very real. In Dr. Guy Leschziner’s new book, “The Nocturnal Brain: Nightmares, Neuroscience and the Secret World of Sleep,” published last month, the renowned neurologist and sleep disorder specialist mentions the possible consequences of untreated sleep apnea. Leschziner is a guest at this year’s Jewish Book Week in London.

“We are now aware that obstructive sleep apnea has a range of long-term implications on our health in terms of high blood pressure, in terms of risk of cardiovascular disease, risk of stroke, impact on cognition and mental clarity,” Leschziner said in an interview with NPR. “And there is now an emerging body of evidence to suggest that actually, obstructive sleep apnea may be a factor in the development of conditions like dementia.”
A poor night’s sleep has the potential to affect our emotional and psychological functioning as well.
How sleep affects mental health is not fully understood, but researchers at the Harvard Medical School have found that sleep problems are an important factor in patients with anxiety, bipolar disorder, depression and attention deficit hyperactivity disorder.
They point to brain imaging and a study of the chemistry of the brain suggesting that a good night’s sleep helps us to bounce back mentally and emotionally to face the challenges of daily living with mental and emotional resilience, while chronic sleep problems can lead to emotional and psychological vulnerability.
Doctors, however, often are not specialists in sleep medicine and get little or no training in sleep disorders, and many patients, like those who suffer from sleep apnea, are hesitant to seek out medical care.
This has been a problem, said Dr. Leibowitz, who practices with the Laureate Medical Group of Northside Hospital. “Often, historically, people have been a little bit embarrassed to talk much about psychiatric problems, and doctors were not reliably asking patients about their sleep and screening for sleep disorders. Although, as we recognize that sleep is a neurobiological process, the options for treatment and evaluation have gotten a lot better.”
Among those choices have been medications. They are part of a class called benzodiazepine, such as Klonopin and zolpidem, which is commonly known as Ambien. Although they have been used in the treatment of insomnia, Dr. Leibowitz doesn’t believe that these powerful medications should be prescribed without a clear understanding of the sleep disorder a patient may have.
“That’s not to say that sleep medications are not helpful and/or effective, but quite honestly, when you treat a symptom without understanding the origin of that symptom, then the treatments are going be less effective and potentially expose the patients to risks. Medications should be used when you understand what you’re treating as opposed to the general complaint of ‘I can’t sleep.’”
Concern about the side effects from long-term use of sleeping medications has led the National Institute of Health to recommend that psychological therapy be considered as an alternative to drugs. This is particularly so in the treatment of insomnia, which is said to affect up to a third of all Americans and result in more than $100 billion dollars in direct and indirect costs.
The use of what is called cognitive behavioral therapy for insomnia also has been endorsed as a first-line therapy by the American Academy of Sleep Medicine. Unlike pills, the program treats the underlying behavioral causes of insomnia rather than just the symptoms. A highly trained therapist, with specialized skills, helps clients to develop good sleep habits and avoid behaviors that keep them from sleeping well.
CBT-I is a structured program of up to a dozen sessions that helps identify and replace thoughts and behaviors that cause or worsen sleep problems with habits that promote sound sleep.
For those who might like to work on their insomnia without the help or expense of a therapist, they can download a free cognitive behavioral training app developed by the U.S. Department of Veterans Affairs. It’s called CBT-i Coach.
For those without serious issues, the National Sleep Foundation offers these tips for a better night’s sleep:
- Stay away from video and computer screens just before bedtime.
- Avoid caffeine in the evening.
- Don’t eat late or drink alcohol at night.
- Put yourself on a sleep schedule that has you going to bed and awakening at the same time each day.
- Keep your bedroom cool and comfortable.
- Check with a sleep specialist if you don’t get much relief. You may need medical treatment.
If you need a doctor’s help, that treatment will be a lot better than it was 30 years ago or more, according to Dr. Leibowitz.
“The body of research in sleep medicine that we have has been evolving dramatically. In just the last few decades it’s like the difference in the general practice of medicine in the 1890s and in the early 1900s to medicine today.”

Greenhut would probably agree. After his sleep improved with the CPAP machine his doctor prescribed, he began exercising on an elliptical machine and totally dropped the fried foods, the sugar and the empty carbs.
In 1 ½ years he’s lost 110 pounds and has improved his health so dramatically his doctor told him he didn’t need to use his sleep machine anymore. Next month he begins his new career as a motivational speaker to convert others to his eating and exercise program and to tell them to get a good night’s sleep.



comments